Ⅰ. Introduction
Malignant extraoral tumors rarely metastasize distantly to the oral cavity.1,2 The primary sites of malignant tumors that metastasize to the oral cavity include the lungs and various areas of the body.1,3,4 Such malignant tumors metastasize to the oral cavity, affecting the gingiva and soft tissues.1,5
Adenocarcinoma, the most common type of lung carcinoma, is characterized by lymphatic and migratory metastases. When lung cancer metastasizes, especially into the oral cavity, it primarily does so to the soft tissues.2 Few studies have reported metastases to peri-implant areas.6,7 Moreover, the presence of dental implants may promote metastasis and metastatic growth, making it challenging to distinguish metastasis from peri-implantitis.8
Patients with a history of extraoral malignancies and symptoms related to peri-implantitis should be screened for metastatic oral malignancies. Since examinations such as bone scans and positron emission tomography–computed tomography (PET/CT) are performed of patients with malignant tumors, they can capture findings pertaining to the regions of the jawbone. In addition, a differential diagnosis based on histopathological examination may be necessary.
This study aimed to report a case of a peri-implant malignant tumor that metastasized distantly from a lung adenocarcinoma to the oral cavity.
Ⅱ. Case Report
A 77-year-old man with hypertension, atrial fibrillation, coronary artery obstructive disease, emphysema-type chronic obstructive pulmonary disease, thrombocytopenia, and non-small cell lung cancer visited our hospital with persistent pain following implant prosthesis removal. The patient was diagnosed with adenocarcinoma by lung biopsy 1 year and 7 months prior to visiting our oral surgery department.
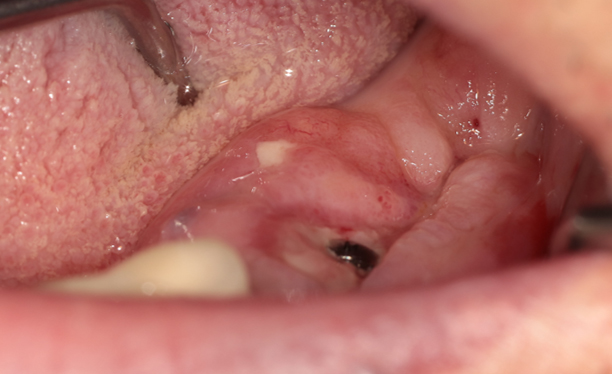
An intraoral examination revealed swelling and slight redness of the left mandibular posterior region impacting the soft tissue of the healing abutment (Fig. 1). Initial panoramic radiography revealed bone loss around the dental implant fixture within the left mandible (Fig. 2).
Peri-implantitis and an abscess due to odontogenic infection were diagnosed and treated with incision and drainage (I&D) and antibiotic therapy. When the patient visited the hospital for drain removal 1 week after the I&D, edema and sustained gingival hyperplasia were observed in the peri-implant area. To ensure a thorough evaluation, a biopsy was planned after the symptoms had alleviated at follow-up (F/U), and an incisional biopsy was performed at the site of gingival thickening 1 week later. The tissue samples were sent to the pathology department for analysis. Immunohistochemical staining was positive for thyroid transcription factor-1. Therefore, the patient was diagnosed with a metastatic adenocarcinoma originating from the lungs.
As surgical management was difficult because of his general condition, we collaborated with the hematology, oncology, and respiratory medicine departments to manage his chemotherapy. Chest CT, abdominal and pelvic CT, brain magnetic resonance imaging, whole-body bone scans, and laboratory tests were performed in the respiratory medicine department, and paclitaxel/carboplatin chemotherapy was planned during the hospitalization. A bone scan performed in the respiratory medicine department before the patient visited the oral and maxillofacial surgery department showed increased uptake in the left mandible. However, the radiology department did not determine the definitive pattern of bone metastasis and confirmed the absence of metastasis to other organs.
Five months later, the patient revisited the hospital with bilateral edema in the midfacial region. No significant findings were observed in this region compared to those from the previous panoramic radiograph (Fig. 3). An intraoral examination revealed gingival swelling, redness, and infection control. After 1 week, the symptoms were alleviated, with no clear signs of infection.
F/U brain magnetic resonance imaging and PET/CT scans were performed by the respiratory medicine department, and an increase in uptake (SUVmax 19.05) (Fig. 4) in the relevant region was identified compared to the uptake in the left mandible (SUVmax 7.41) observed on PET/CT taken 1 year prior. Moreover, lymph node enlargement was observed in the Level 1 area of the left neck. Local radiation therapy (RTx) of the left mandible and neck was planned to control pain caused by the carcinoma. Subsequently, intensity-modulated radiation therapy (IMRT) with a total of 5600 cGy (Centi Gray) at 2 Gy/fraction was performed for 1 month at our hospital’s radiation oncology department.
Three months after the hospitalization for chemotherapy, the patient was referred to our department with persistent intraoral bleeding, but no significant difference was noted in panoramic imaging findings from the previous panoramic images. An intraoral examination showed that ulcerative lesions and crusts had formed on the left buccal mucosa, lips, and tongue, causing repeated bleeding even with mild stimulation. A hematoma removal was performed and follow-up continued, with ulcer-like lesions remaining despite hematoma and pseudomucosa removal. Thereafter, a bone scan was performed during the F/U in the respiratory medicine department, and increased uptake was observed in the left mandibular region (Fig. 5).
Two months later, the patient exhibited signs of tissue necrosis in the lesion and revisited our department for antibiotic therapy (Fig. 6). Afterward, when he was hospitalized for chemotherapy administration, an intraoral examination showed that the ulcers and necrotic tissue in the left mandibular molar region had decreased compared with the previous visit. Hence, follow-up was planned once the pain was controlled.
Four months later, the patient visited the hospital with an exposed dental implant fixture in the oral cavity. The dental implant abutments were more exposed to the oral cavity without necrotic tissue than those in the first oral surgery department visit. The tumor size was partially reduced (Fig. 7). Afterward, the implant fixture continued to be exposed, and the patient complained of discomfort; therefore, the abutment overlying the implant was removed and the patient was followed up. Subsequently, no significant changes were observed in the metastatic carcinoma of the oral cavity, the soft tissue thickening was reduced, and the mandibular resorption had advanced slightly (Fig. 8).
Ⅲ. Discussion
Malignant tumors from body parts other than the oral cavity rarely metastasize distantly to the oral cavity.3,9 The present case involved metastasis to a dental implant site. In particular, metastatic malignant tumor lesions are not easy to distinguish solely from intraoral findings and difficult to differentiate from peri-implantitis. Overall, alveolar bone loss was similar to the alveolar bone resorption pattern that occurs after general tooth extraction. Clinically, the extensive thickening of the gingival area toward the left mandibular molar area is different from the general symptoms of adult periodontitis. However, since no lumps or ulcers were observed, it was difficult to differentiate it as a tumor-like lesion based solely on the condition of the oral mucosa.
Primary carcinomas that metastasize to the oral cavity are often lung adenocarcinomas.10 Even in cases of peri-implant metastasis, the primary cancer is often lung adenocarcinoma.7,8,11 Gingival metastasis indicates a poor prognosis. Malignant tumors of the oral cavity caused by distant metastases are rare. Moreover, oral metastasis accounts for a low percentage of all oral cancers.12 Primary sites include the lungs, kidneys, skin, breast, liver, bone tissue, rectum, stomach, small intestine, and ovaries in women.1, 2, 3,6 When such malignant tumors metastasize to the oral cavity, the metastatic sites include the gingiva, tongue, tonsils, palate, lips, floor of the mouth, buccal mucosa, uvula, and vestibular region.1, 2, 3,8
Distant metastases to the oral cavity, as in this case, can be treated with radiotherapy or chemotherapy; in some cases, they can even be removed surgically. In the present case, surgery was not an option because of the patient’s general condition; however, IMRT was performed. After IMRT, the tumor size decreased. Although osteoradionecrosis did not occur in this case, its possibility must be considered in cases of implant removal and intraoral prosthetic treatment.13 There is little literature on RTx for malignant tumors around implants, such as in this case. However, irradiation of the implant with more than 40 Gy during RTx in patients with head and neck cancer can act as a risk factor for alveolar bone loss around the implant.14
The prognosis after implant placement in the irradiated area showed an average survival rate of approximately 87.8%, significantly different from non-irradiated implants.15 A lower dental implant survival rate was observed with irradiation exceeding 50 Gy. Consensus is lacking regarding implant placement after RTx. Considering that revascularization and new bone formation occur 3–6 months after radiation treatment, dental implants are sometimes recommended 6–12 months or 6–18 months later.16
Clinicians find it difficult to distinguish between early peri-implant malignancies and peri-implantitis. When only bone loss is observed without symptoms, it is difficult to determine whether a tumor or peri-implantitis causes the bone loss. However, if a history of malignant tumors is confirmed as in this case, peri-implant malignancy due to distant metastasis should be suspected. Therefore, a histopathological examination is required for differentiation.
Patients with a history of malignant tumors have undergo imaging such as bone scans and PET/CT for diagnosis, which can help evaluate the jawbone area.17 In this case, bone scans showed an increase in uptake of the left mandible compared to the PET/CT scan taken 2 years prior to the oral surgery department visit (Fig. 9). The uptake might have increased because of periodontitis or peri-implantitis; however, considering the clinical findings, the possibility that the tumor had metastasized cannot be excluded. Moreover, according to the PET scan performed 6 months before the patient’s visit to the oral surgery department, the SUVmax was 7.41 in the posterior region of the left mandible, indicating increased uptake. The SUVmax of patients with dental problems such as periodontitis and periapical disease is generally approximately 2.4–5.6.17 As the possibility of a dental problem caused by another disease could not be excluded in this case, a dental evaluation was deemed necessary.
Several studies have reported that chronic inflammatory conditions may affect malignant tumor development.8,18,19 With less clear evidence, claims have been made that the presence of implants can promote cell metastasis and metastatic growth.8 The peri-implant area is more vulnerable to infection than is the area around natural teeth, which is more likely to remain in a chronic inflammatory condition. The I&D performed when the patient first visited the dentist may have influenced the tumor spread.
In this case, a dental evaluation was performed after the onset of infective symptoms. In other words, because it is difficult for patients to recognize peri-implant disease, the evaluation itself may be delayed. Additionally, in the early stages, peri-implantitis and similar tumors are asymptomatic, making it difficult for dentists to recognize them.6,7,20
Diagnosis based solely on clinical and radiological evidence is difficult and requires a biopsy. PET/CT and bone scans can aid the diagnosis, as in this case, a suspicious lesion existed in the oral cavity.17,19 However, to prevent delays in appropriate treatment, a tissue biopsy must be considered.
It is necessary to consider problems that may occur after implant placement. Furthermore, patients with a history of malignant tumors require careful diagnosis and treatment, particularly those with irradiated jawbones.13
Ⅳ. Conclusion
Clinicians find it challenging to diagnose malignancies that mimic peri-implantitis around dental implants. If the intraoral symptoms of patients with extraoral malignant lesions are similar to those of peri-implantitis, if the oral soft tissue differs from the typical alveolar bone loss occurring after dental extractions, or if mucosal thickening is observed, a tissue biopsy is required to ensure diagnostic accuracy. This case report demonstrates that radiation osteonecrosis should be considered during dental implantation.